

The human body constitutes nearly an average of 5 liters blood in the body. Composed of about 55% fluid plasma, the remaining part of the blood is constituted of blood cells and platelets. Blood plasma is the liquid component of the blood formed primarily of water, also comprising of essential dissolved proteins, organic and inorganic substances. Also, the different types of blood cells in the body perform integral functions enhancing the efficiency of the circulatory system. The red blood cells or erythrocytes are associated with oxygen transport in association with hemoglobin from the lungs to the different parts of the body and in the removal of carbon dioxide from the different body tissues and the lungs. White blood cells or leucocytes contribute to the defense and repair mechanisms of the body. Blood platelets or thrombocytes enable blood coagulation and clotting.
Our blood type and blood groups have been categorized on the basis of the presence of specific antigens and antibodies. Antigens are blood group determinants present on the cellular surface of the RBCs. Antibodies are protein molecules in the blood plasma which is capable of eliciting an immune response against any foreign molecule in the blood. Although, there are 35 internationally established blood group or type classification systems, there are two most widely applied classifications of blood group which has been discussed in the subsequent paragraphs.
ABO BLOOD GROUPS:
This system of classification defines four different blood groups- A, B, AB and O. The blood group of an individual is an outcome of genetic inheritance from their parents. Whether it is A, B, AB or O, our blood groups are completely influenced by the blood types of our parents.
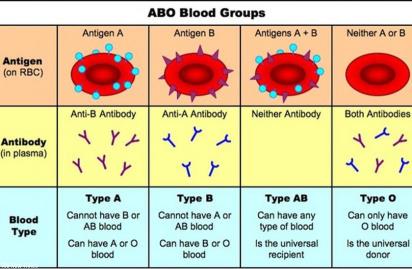
Characteristics of the ABO blood groups
• Blood group A: Characterized by the presence of antigen A on the surface of RBCs and anti-B antibodies in the blood serum.
• Blood group B: Characterized by the presence of antigen B on the surface of RBCs and anti-A antibodies in the blood serum.
• Blood group AB: Characterized by the presence of both antigens A and B on the surface of RBCs without any antibodies in the blood serum.
• Blood group O: Characterized by the absence of both antigens A and B on the surface of RBCs but with the presence of both anti-A and anti-B antibodies in the blood serum.
Significance of ABO System
• Blood transfusion: Before a transfusion is performed, the blood group compatibility between the donor and the recipient is to be examined to ensure the safety of the clinical procedure. Generally, in the situation of an incompatibility, the transfusion reaction is triggered which might cause the disruption of the recipient RBCs and could bear fatal results. For instance, when the patient or the recipient with blood group A receives a blood transfusion from a donor with blood group B, a transfusion reaction owing to incompatibility will result. The donor has surface antigens B on its RBCs and anti-A antibodies in their blood serum. However, the recipient has surface antigen A and anti-B antibodies in their blood serum. Thus, when the recipient with blood group A receives blood from the donor with blood group B, the donor anti-A antibodies agglutinates the recipient’s A antigens , thereby causing rupture of RBCs also known as hemolysis, which is capable of causing death.
• Universal donor and Universal recipient: People with blood group O are called universal donors, owing to the absence of either antigen A or B from the surface of their RBCs, with the presence of both anti-A and anti-B antibodies in their blood serum. Thus, effectively used for blood transfusion. However, people with blood group AB with both surface antigen A and B in their RBCs but no antibodies in their blood serum are thus, universal recipients since the risks of transfusion reaction are low in this case. But, they are capable of donating blood only to recipients with AB blood group exclusively.
• Plasma compatibility: The blood plasma of donors with O blood group contain both the antibody, anti-A and anti-B, thus, are capable of receiving plasma from any blood group but can donate the same to recipients with O type plasma. On the contrary, blood plasma donors with AB blood group do not contain either antibody, anti-A or anti-B, thus, are capable of donating plasma to recipients of any blood group but receive it from only a donor of AB blood group. Thus, plasma compatibility is the exact opposite of the compatibility testing in case of blood transfusion.
• Bombay blood group: The precursor of antigen A and B on the cellular surface of RBCs is the H antigen which converts to either A or B antigen thereby, determining the blood group of an individual. Though, not exactly as part of ABO system of blood groups, there could be an incidence of an extremely rare blood group among people ie. the Bombay blood group. The inability of the H surface antigen on the RBC into either antigen A or antigen B results in this blood type. Due to the absence of either antigen A and B in their RBCs, people with this blood group are capable of donating blood to recipients with any blood type but can receive blood from donors with the Bombay blood group exclusively.
• Blood group genotyping: Through studies based on the molecular basis of known antigens, an extensive description of the blood group of individuals can be determined and thus, the correct match for the recipient undergoing blood transfusion can be identified.
RHESUS BLOOD GROUPS:
Other than A or B antigens on the surface of RBCs, is the possibility of the presence or absence of a Rhesus factor or RhD antigen. This means that the Rh factor could either be present ie. the individual could be Rhesus-positive (Rh +) or be absent ie. the individual could be Rhesus-negative (Rh -). Unlike ABO antigens, antibodies are produced against the Rh factor through blood transfusion or placental sensitization. Nearly 85-93% of human beings are Rhesus positive. The Rhesus factor influences the classification of blood types into eight different blood groups as follows:
• A+
• A-
• B+
• B-
• O+
• O-
• AB+
• AB-
Significance of the Rhesus factor
• Hemolytic disease of the fetus and newborn: In the case of pregnancy, when the mother is Rh-negative while the fetus inherits the Rh factor from the father, there is a risk to the health of the fetus due to the impact of the mother’s antibodies in disrupting the fetus RBCs. This clinical condition is referred to as the hemolytic disease of the fetus and newborn (HDFN).
Rhesus disease may lead to anemia and jaundice among newborns while causing no such harm to the mother. Because the mother is Rh negative, the risks of this disease occurring in the fetus is accentuated, through the sensitization of the mother on prior exposure to the Rh+ blood possibly due to a previous pregnancy with a Rh+ fetus. If prior sensitization takes place before, the woman’s body automatically elicits an immune response by producing antibodies against the foreign fetal cells which are Rh+ causing HDFN.
The incidence of Rhesus disease has become a rarity due to the advent of medicine. Intravenous injections of anti-RhD antibodies can be administered in the mother’s body during pregnancy to help remove Rh-positive fetal cells preventing sensitization.
• Blood transfusion: Cross-matching of blood phenotypes between the donor and recipient becomes integral for performing an effective blood transfusion. Rh- recipients with anti-RhD antibodies in their blood can receive a transfusion from Rh+ donors, however , this would cause sensitization of the donor to the Rh antigen.

RHESUS COMPATIBILITY CHART
According to some ancient mythological beliefs, it is believed that other than being representative of one’s blood group, the ABO system defines the personality traits and compatibility between individuals. These beliefs marked the origin of racial discrimination and related complications in spite of this being just a scientific basis for blood type classification.
